
(908) 381-8160Berkeley Heights

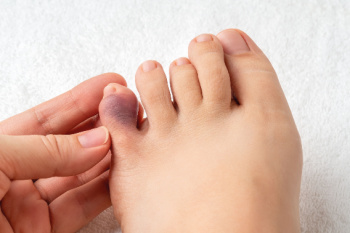
A broken pinky toe often occurs from direct trauma, such as stubbing the toe against furniture or dropping a heavy object on the foot. It can also result from repetitive stress or overuse during physical activities that place pressure on the feet. Individuals with weakened bones or poor footwear support may be more susceptible. Symptoms of a broken pinky toe include sharp or throbbing pain, swelling, and visible bruising. The toe may appear crooked or misaligned, and walking can become difficult due to discomfort or instability. In some cases, the pain may persist even at rest. If you have broken your pinky toe, it is suggested that you promptly contact a podiatrist who can offer you appropriate treatment solutions.
A broken toe can be very painful and lead to complications if not properly fixed. If you have any concerns about your feet, contact Dr. Janet Leicht from New Jersey. Our doctor will treat your foot and ankle needs.
What to Know About a Broken Toe
Although most people try to avoid foot trauma such as banging, stubbing, or dropping heavy objects on their feet, the unfortunate fact is that it is a common occurrence. Given the fact that toes are positioned in front of the feet, they typically sustain the brunt of such trauma. When trauma occurs to a toe, the result can be a painful break (fracture).
Symptoms of a Broken Toe
Generally, it is best to stay off of the injured toe with the affected foot elevated.
Severe toe fractures may be treated with a splint, cast, and in some cases, minor surgery. Due to its position and the pressure it endures with daily activity, future complications can occur if the big toe is not properly treated.
If you have any questions please feel free to contact our office located in Berkeley Heights, NJ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
The forefoot is composed of five metatarsal bones and fourteen phalanges. Each toe has three phalanges except for the big toe which only has two. Our toes play an essential role to the walking process, which is why a broken toe could seriously disrupt one’s ability to move around. Toe fractures are common and can be very painful. Fortunately, these injuries rarely require surgery and usually heal with rest and a change in activity.
Broken toes typically result from a traumatic event such as falling, stubbing the toe, or dropping something on the toe. Traumatic toe fractures may be categorized as either minor or severe fractures. At times, one may hear a “pop” or “crack” sound when the bone breaks. Common symptoms of a traumatic toe fracture include pain, throbbing, bruising, swelling, and redness.
Another type of toe fractures is a stress fracture. These injuries usually appear in the form of small hairline breaks on the bone. Stress fractures develop after repetitive activity instead of a single injury. Stress fractures occur when the muscles in the bone become too weak to absorb impact. Consequently, the toe bone becomes vulnerable to any pressure and impact it endures. Symptoms for a stress fracture in the toe include swelling without bruising, tenderness to the touch, pain that goes away with rest, and pain after walking or running.
If you suspect that you have a broken toe, you should make an appointment with your podiatrist. He or she will likely diagnose you by performing a physical exam and an X-ray. Treatment for a broken toe may include the R.I.C.E. method, buddy taping, surgery, or antibiotics. The R.I.C.E. method (Rest, Ice, Compression, and Elevation) is a common treatment method for many injuries because it decreases pain. Buddy tapping involves wrapping the injured toe next to an adjacent toe to keep it supported and protected. These two methods have proven to be effective in the healing process for toe fractures. The estimated healing time for a broken toe is approximately four to six weeks. If the injury becomes infected or requires surgery, the estimated healing time may take eight weeks or more.
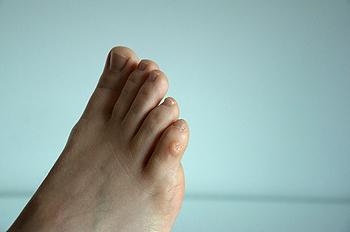
Corns are thickened areas of skin that usually develop on or between the toes as the result of constant pressure or friction. Corns on the toes or feet can make walking difficult and painful, especially when the affected area rubs against the inside of your shoe. A defining feature of a corn is its hardened core, which can press into the deeper layers of skin and cause sharp pain or tenderness that limits mobility. Symptoms may include dry, flaky skin, discomfort when wearing shoes, and raised, rough bumps that are painful to the touch. Poorly fitting footwear is a common cause of corns, especially styles that crowd the toes or create pressure points. A podiatrist can provide treatment to safely remove a corn as well as suggest prevention strategies. If you have foot pain that is caused by a corn, it is suggested that you schedule an appointment with a podiatrist for an exam and appropriate treatment.
If you have any concerns regarding your feet and ankles, contact Dr. Janet Leicht of New Jersey. Our doctor will treat your foot and ankle needs.
Corns: What Are They? and How Do You Get Rid of Them?
Corns can be described as areas of the skin that have thickened to the point of becoming painful or irritating. They are often layers and layers of the skin that have become dry and rough, and are normally smaller than calluses.
Ways to Prevent Corns
There are many ways to get rid of painful corns such as wearing:
Treating Corns
Treatment of corns involves removing the dead skin that has built up in the specific area of the foot. Consult with Our doctor to determine the best treatment option for your case of corns.
If you have any questions please feel free to contact our office located in Berkeley Heights, NJ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Corns are thickened areas on the skin’s surface, to the point of being irritating and sometimes painful. Commonly found on the feet, corns are circular or cone-shaped. They develop where there are areas of pressure or friction, such as on the little toe when it rubs up against shoes, or on the ball of your foot.
Corns are often confused with a callus, but there is a difference between them. Corns can be raised bumps that are painful to the touch. They consist of a rough, thick area of skin that may be dry or waxy. Corns tend to be surrounded by skin that is inflamed, and are usually much smaller than calluses.
Removing the dead skin that has built up is the key in treating corns. Salicylic acid medication is most common in accomplishing this. The acid works by dissolving keratin, which is the protein that makes up the majority of corns. You can purchase salicylic acid over-the-counter in products such as wart removers. It comes in a variety of forms such as medicated pads, drops, or creams. However, people who are diabetic should not use salicylic acid, but should instead consult their doctor immediately.
According to the product directions, applying the medication directly onto the corn will treat it. The top layer of the corn will begin to turn white after use. When that occurs, the layers of skin can then be peeled away, making the corn smaller. Shaving off corns with razors or other pedicure equipment is never a good idea. This can lead to infection. If your corn gets infected, and is not treated immediately, a visit to the doctor will be necessary.
Another way to treat corns and help prevent their return is by using orthotic inserts, fitted by a podiatrist. Inserts fit right into your shoes and adjusts the way your foot fits into your shoes. This fixes the way you walk. This will lower your chances of getting corns, and eliminate current corns by reducing rubbing from friction.
Surgery is rarely used to treat corns, but does occur on occasion. Surgery actually deals with the underlying issue that causes corns. During surgery, the bone is shaved and any abnormalities are corrected, thus reducing the amount of friction that occurs during walking.
To prevent corns, the first step is reducing friction. Always wear shoes that fit well and don’t rub your feet. Pads can be purchased if you notice rubbing developing. These pads can be purchased over-the-counter, and can be simply placed on the irritated area. Wearing cushioned insoles in your shoes can always reduce the friction, and making sure to wear well-fitting shoes. This will ensure that your foot is not being squeezed awkwardly, and prevent corns from forming in the first place.

Falling can cause significant injuries to the feet, including sprains, fractures, and bruising. Impact from a fall may weaken the muscles and joints, leading to instability and discomfort. Strengthening the feet can help prevent falls by improving balance and stability. Using a resistance band to perform foot exercises enhances flexibility and strengthens the muscles that support the arches. Picking up marbles with the toes helps improve dexterity and grip strength, making the feet more responsive to changes in terrain. Regular stretching and strengthening exercises increase foot control, reducing the risk of missteps. Wearing supportive footwear and maintaining strong, flexible feet contribute to better stability. If you have fallen and have sustained a foot or ankle injury, it is suggested that you promptly visit a podiatrist who can treat various foot conditions.
Preventing falls among the elderly is very important. If you are older and have fallen or fear that you are prone to falling, consult with Dr. Janet Leicht from New Jersey. Our doctor will assess your condition and provide you with quality advice and care.
Every 11 seconds, an elderly American is being treated in an emergency room for a fall related injury. Falls are the leading cause of head and hip injuries for those 65 and older. Due to decreases in strength, balance, senses, and lack of awareness, elderly persons are very susceptible to falling. Thankfully, there are a number of things older persons can do to prevent falls.
How to Prevent Falls
Some effective methods that older persons can do to prevent falls include:
Falling can be a traumatic and embarrassing experience for elderly persons; this can make them less willing to leave the house, and less willing to talk to someone about their fears of falling. Doing such things, however, will increase the likelihood of tripping or losing one’s balance. Knowing the causes of falling and how to prevent them is the best way to mitigate the risk of serious injury.
If you have any questions, please feel free to contact our office located in Berkeley Heights, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Elderly Americans are very susceptible to falls as they get older. Everyone experiences decreases in flexibility, balance, strength, and the senses as they age. This correlates to some eye-opening statistics. 1 in 4 Americans aged 65 and older fall each year. An elderly American is being treated for a fall in an emergency room every 11 seconds. In light of these striking statistics, one can see the importance of taking steps to prevent falls.
Finding an exercise program for the elderly is an excellent way to reduce the likelihood of falls. Look for an exercise program that improves strength and balance. Elderly people who live a more sedentary lifestyle, with little physical activity, are at an increased risk of falling. Wearing well-fitted footwear that provides good foot support and cushion will help prevent falls from poorly fitted shoes. Talking to a podiatrist about your susceptibility to falls and about inspecting your prescriptions will help to avoid any medication that could make falls more likely. Due to a decline in the senses among the elderly, having your eyes and hearing checked is recommended.
Around half of all falls occur in the household. Removing tripping hazards in the home and making it more accommodating to older persons can significantly reduce falls. Some notable household changes include increasing lighting around the house, installing grab bars in the shower and bathroom, and making sure the floor is clear of clutter. Other smart options include installing a shower chair, using rubber-bottomed rugs, and placing railings on both sides of stairwells.
Finally, discuss with a doctor and your family about your fear of falling. This will help to increase awareness among the population on the need for fall prevention. A lack of awareness on the matter, and a downplaying of importance are what increase the risks of falling. Following these tips can help to reduce the risk for yourself and your loved ones.
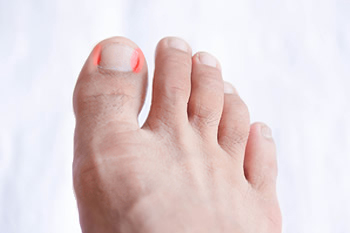
Ingrown toenails occur when the edges of a toenail grow into the surrounding skin, causing pain, swelling, and redness. This condition most commonly affects the big toe and can result from improper nail trimming, wearing tight shoes, or trauma to the toe. In some cases, ingrown toenails can develop due to fungal infections or genetic factors. Symptoms include sharp pain, tenderness, and swelling surrounding the affected toenail. In more severe cases, an infection may develop, leading to pus or discharge from the area. The toe may appear red or inflamed, making wearing shoes or walking uncomfortable. A podiatrist can diagnose and treat ingrown toenails through various methods, such as recommending proper nail care, prescribing antibiotics for infections, or performing minor surgery to remove the ingrown portion of the nail. If you have a painful ingrown toenail, it is suggested that you schedule an appointment with a podiatrist, who can provide appropriate treatment solutions.
Ingrown toenails may initially present themselves as a minor discomfort, but they may progress into an infection in the skin without proper treatment. For more information about ingrown toenails, contact Dr. Janet Leicht of New Jersey. Our doctor can provide the care you need to keep you pain-free and on your feet.
Ingrown Toenails
Ingrown toenails are caused when the corner or side of a toenail grows into the soft flesh surrounding it. They often result in redness, swelling, pain, and in some cases, infection. This condition typically affects the big toe and may recur if it is not treated properly.
Causes
You are more likely to develop an ingrown toenail if you are obese, have diabetes, arthritis, or have any fungal infection in your nails. Additionally, people who have foot or toe deformities are at a higher risk of developing an ingrown toenail.
Symptoms
Some symptoms of ingrown toenails are redness, swelling, and pain. In rare cases, there may be a yellowish drainage coming from the nail.
Treatment
Ignoring an ingrown toenail can have serious complications. Infections of the nail border can progress to a deeper soft-tissue infection, which can then turn into a bone infection. You should always speak with your podiatrist if you suspect you have an ingrown toenail, especially if you have diabetes or poor circulation.
If you have any questions, please feel free to contact our office located in Berkeley Heights, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
An ingrown toenail is a nail that has curved downward and grown into the skin. This typically occurs at either the nail borders or the sides of the nail. As a result, pain, redness, swelling, and warmth may occur in the toe. If a break in the skin forms due to the ingrown nail, bacteria may enter and cause an infection in the area; this is typically characterized by a foul odor and drainage.
Ingrown toenails have multiple reasons for developing. In many instances, the condition is a result of genetics and is inherited. The most common cause, however, is improper trimming; cutting the toenails too short forces the skin beside the nail to fold over. An ingrown toenail can also develop due to trauma, such as stubbing the toe, having an object fall on the toe, or participating in activities that involve repeated kicking or running. Wearing shoes that are too tight or too short can also cause ingrown toenails.
Treatment for an ingrown toenail varies between patients and the severity of the condition. In most cases, it is best to see your podiatrist for thorough and proper treatment. After examining your toe, your podiatrist may prescribe oral antibiotics to clear the infection if one is present. Surgical removal of either a portion of the nail or the entire nail may also be considered. In some cases, complete removal or destruction of the nail root may be required. Most patients who undergo nail surgery experience minimal pain afterward and can return to normal activity the following day.
Ingrown toenails can be prevented with proper nail trimming and by avoiding improper-fitting shoes. When cutting the toenails, be sure that you are cutting in a straight line and avoid cutting them too short. Shoes should not be too short or tight in the toe box.
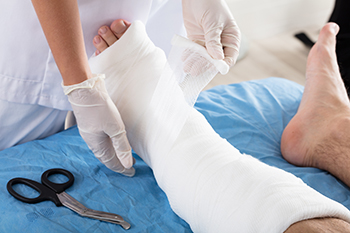
Total contact casts are extremely effective for managing diabetic foot ulcers, particularly those caused by neuropathy. These casts distribute pressure evenly across the foot and ankle, to reduce stress on the ulcerated area and promote healing. By immobilizing the foot, a total contact cast also limits excessive movement, which can further aggravate wounds. Total contact casts ensure consistent pressure relief since patients cannot remove them, leading to higher healing rates. These casts are particularly beneficial for non-infected ulcers where circulation remains adequate. While total contact casts offer significant advantages, they require careful monitoring to prevent complications like skin irritation or new pressure points. A podiatrist can assess whether a total contact cast is appropriate based on wound severity, circulation, and overall foot health. Regular evaluations are needed to ensure proper healing and adjust the cast. If you are experiencing foot problems related to diabetes, it is suggested that you schedule an appointment with a podiatrist to see if a total contact cast is right for you.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact Dr. Janet Leicht from New Jersey. Our doctor can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact our office located in Berkeley Heights, NJ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.